The Best Intermittent Fasting Protocols For Women Who Want Sustainable Weight Loss
Mark Mattson, Ph.D.
Neuroscientist, Johns Hopkins University
Fasting prolongs the period where your body exhausts sugar stores and begins burning stored fat for fuel — and the benefits extend well beyond weight loss.
Summary (TL;DR)
This guide to intermittent fasting (IF) focuses on women's unique needs, as most research centers on men. IF, especially the 16/8 method, can improve insulin sensitivity and trigger beneficial autophagy. Unlike rigid daily fasting, this guide emphasizes cycle-syncing, adjusting fasting to match a woman's menstrual phase for better results. Those pregnant, nursing, or with certain health conditions should seek medical advice. IF is an eating pattern focused on timing, not a restrictive diet.
Most intermittent fasting guides are built on research done primarily with men, then handed to women with a quiet assumption that it applies equally. A lot of the time, it doesn't.
Here's what's actually true: IF can work remarkably well for women. The 16/8 method improves insulin sensitivity. Fasting-triggered autophagy — the cellular cleanup process that earned Yoshinori Ohsumi the 2016 Nobel Prize — is real and accessible without extreme protocols. The research on PCOS-related androgens is genuinely promising.
But the version of intermittent fasting most guides recommend — rigid, daily, same window every day — ignores the 28-day hormonal cycle that governs how a woman's metabolism actually operates. That gap is why so many women try IF, push hard for six weeks, see mixed results, and conclude it doesn't work for them.
It does work. It just needs to be done differently.
This guide covers the science, the four main methods, the honest hormone story (including the parts most articles skip), and a cycle-syncing framework that adjusts fasting intensity to where you actually are in your cycle.
Medical & Referral Disclaimer
The content in this article is for educational purposes only and does not constitute medical advice. Intermittent fasting affects individuals differently based on hormonal status, health history, age, and lifestyle factors. Women who are pregnant, breastfeeding, under 18, diabetic, underweight, or have a history of eating disorders should not practice intermittent fasting without direct medical supervision. If you experience irregular periods, significant fatigue, hair loss, or worsening mood while fasting, stop the protocol and consult your healthcare provider. Always seek professional medical guidance before starting any new dietary practice, especially if you are managing a hormonal condition, thyroid disorder, or taking prescription medication.
Key Takeaways
- Intermittent fasting is an eating pattern, not a diet. It focuses on when you eat, not what.
- The 16/8 method is the most studied and most sustainable starting point for women.
- Fasting triggers the metabolic switch from glucose to fat burning at roughly the 12-hour mark.
- A 2022 review of human trials found IF reduces testosterone by 9–26% in women with PCOS — a clinically significant result.
- Short-term time-restricted eating does not significantly change estrogen or progesterone in healthy women.
- Aggressive fasting can elevate cortisol, suppress GnRH signaling, and disrupt the menstrual cycle — particularly in the luteal phase.
- Cycle-syncing your fasting window (adjusting length by menstrual phase) produces better results with fewer side effects than a fixed daily protocol.
- Women who are pregnant, nursing, diabetic, under 18, or have a history of eating disorders should not practice intermittent fasting.

What Is Intermittent Fasting?
Intermittent fasting is an eating pattern that cycles between defined periods of fasting and eating. It does not restrict what you eat — only when. The most common approach, the 16/8 method, involves fasting for 16 hours and eating within an 8-hour window each day.
This distinction matters. IF is not a diet in the traditional sense. It doesn't require calorie counting, food elimination, or special products. What it does require is managing eating timing consistently, which turns out to have real metabolic consequences independent of food choices — though food quality inside the eating window matters a great deal.
Several protocols fall under the intermittent fasting umbrella. They range from daily time-restricted eating to multi-day or weekly fasting approaches, and the evidence behind each varies significantly.
How Intermittent Fasting Works: The Metabolic Switch
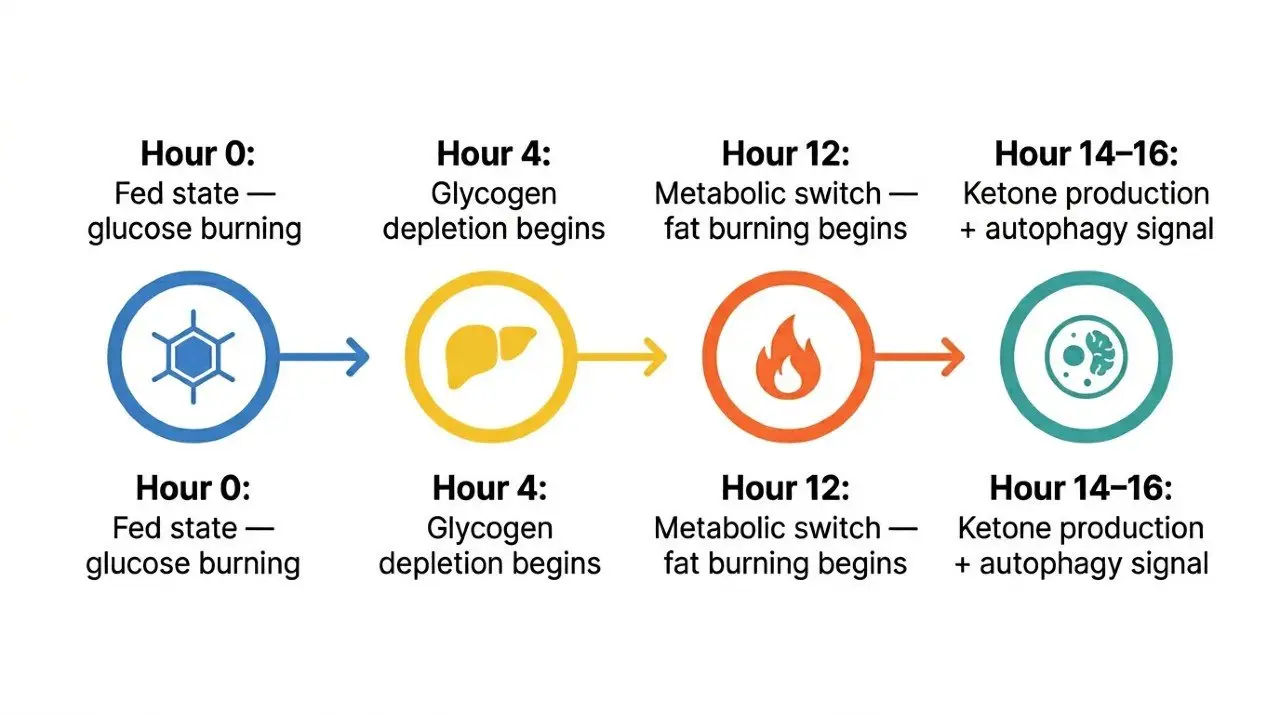
When you stop eating, your body burns through glucose stores first. After roughly 12 hours without food, liver glycogen is depleted, and your metabolism shifts to burning stored fat for energy. This is the metabolic switch.
That switch produces ketones — primarily beta-hydroxybutyrate — which the brain uses readily as an alternative to glucose. According to Mark Mattson, Ph.D., a neuroscientist at Johns Hopkins, "fasting prolongs the period where your body exhausts these sugar stores and begins burning stored fat for fuel." The metabolic benefits compound with fasting duration, up to a point.
For women, that "up to a point" matters. The hormonal costs of prolonged fasting are real and worth understanding before going further.
Autophagy: The Nobel Prize-Winning Reason Fasting Goes Beyond Weight Loss
Autophagy is the body's cellular cleanup process. During a fast, cells begin breaking down and recycling damaged proteins, malfunctioning organelles, and cellular debris — essentially a biological reset.
Yoshinori Ohsumi won the 2016 Nobel Prize in Physiology or Medicine for mapping the genetic mechanisms that control this process. Before his work, fewer than 20 papers per year mentioned autophagy. Today, more than 5,000 studies are published annually, covering their links to inflammation, metabolic disease, cognitive decline, and longevity.
Practically, autophagy begins meaningfully around the 12–16 hour fasting mark. The 16/8 method just touches the threshold by the end of each fasting window — enough to trigger the signal, not a deep cellular dive. Women who extend to 18 hours occasionally (not daily) may capture stronger autophagy benefits without the sustained hormonal disruption that comes with frequent long fasts.
Brain Benefits: BDNF And The Cognitive Case For Fasting
Fasting increases Brain-Derived Neurotrophic Factor (BDNF), a protein that supports the growth and maintenance of neurons and protects against cognitive decline. Ketones from fasting also provide the brain with a clean, steady fuel source that bypasses the blood sugar fluctuations responsible for afternoon brain fog.
Many women report unusually clear thinking during fasting periods. This is why. It's not a placebo — it's BDNF and metabolic fuel switching working together.
The 4 Main Intermittent Fasting Methods
| Method | Fasting Window | Eating Window | Difficulty | Best Fit |
|---|---|---|---|---|
| 16/8 (Time-Restricted Eating) | 16 hours daily | 8 hours daily | Moderate | Beginners, daily practice |
| 5:2 Protocol | 500–600 cal, 2 days/week | Normal eating 5 days/week | Moderate | Weekly flexibility preference |
| Alternate-Day Fasting | Every other day | Every other day | High | Advanced practitioners |
| 24-Hour Fast | Full 24 hours | Normal eating other days | High | Experienced fasters only |
The 16/8 Method
The 16/8 method is the most researched intermittent fasting protocol and the easiest to maintain long-term. Eat within an 8-hour window — say, noon to 8 pm — and fast for the remaining 16 hours. Skipping breakfast extends the natural overnight fast without adding much deliberate restriction, which makes this feel less like a diet and more like a schedule shift.
For women starting with IF, this is the logical entry point. It's conservative enough to preserve hormonal stability while still triggering the metabolic switch and reaching the early threshold of autophagy.
The 5:2 Protocol
Two days per week, intake is limited to 500–600 calories. The other five days are unrestricted. Research documented in a 2024 PMC review on IF and hormonal regulation shows the 5:2 approach produced a 50% reduction in insulin levels and measurably decreased insulin resistance (HOMA-IR). That's a significant metabolic result, particularly for women managing PCOS or metabolic syndrome.
The catch: women's energy needs change across the menstrual cycle. Attempting a 500-calorie day during the luteal phase — when progesterone raises baseline caloric needs by 100–300 calories — can spike cortisol and trigger rebound eating. Scheduling the 5:2 restricted days during the follicular phase largely solves this problem.
Alternate-Day Fasting
This protocol alternates normal eating days with restricted days (500–600 calories or full fasting). The metabolic effects are similar to 5:2, but the day-to-day demands are harder to manage, particularly around workouts, social eating, and cycle-related energy shifts. Most women find daily 16/8 more sustainable than alternate-day fasting for the same results.

24-Hour Fasts
Complete fasting once or twice weekly (the "Eat Stop Eat" approach). The autophagy stimulus is stronger than shorter windows. The hormonal risk is also higher: extended fasting can suppress GnRH (gonadotropin-releasing hormone), the signal that regulates estrogen and progesterone production. Frequent 24-hour fasts are not a good match for most premenopausal women unless done strategically during the follicular phase and infrequently.
What Intermittent Fasting Actually Does To A Woman's Body
The honest answer is: it depends on your hormonal state, your life stage, your fasting duration, and what you eat in your eating window. Here's what the current evidence shows.
Fat Loss And Insulin Sensitivity
The headline results are real. The PMC review on IF and hormonal regulation documented 50% reductions in insulin levels from both alternate-day fasting and 5:2 over as few as 22 days. Early time-restricted feeding improved insulin sensitivity and reduced fasting plasma glucose over five weeks.
Fat loss from IF is real but modest in clinical trials — roughly 2–4% body weight over 8–12 weeks on time-restricted eating. Effects are stronger when calories are consumed earlier in the day rather than in the evening. The combination of IF with adequate protein and resistance training produces better body composition outcomes than IF alone.
Hormonal Effects: The Part Most Articles Skip
The research on IF and women's hormones is more nuanced than most sources acknowledge, and that nuance matters. Here's the full picture.
How Intermittent Fasting Affects Women's Hormones
| Hormone | Short-Term Fasting Effect | Sustained Effect | Clinical Significance |
|---|---|---|---|
| Insulin | ↓ 50% (5:2 and ADF protocols) | Improved sensitivity | High benefit |
| Estrogen / Progesterone | Minimal change with moderate TRE | Can disrupt with aggressive/calorie-restricted fasting | Moderate risk |
| Testosterone / FAI | ↓ 9–26% in PCOS (especially with early eating) | Beneficial for androgen excess | High benefit for PCOS |
| DHEA | ↓ 13–14% in 8 weeks | Remains within normal range | Low risk, monitor long-term |
| Cortisol | ↓ with non-restrictive TRE; ↑ with caloric restriction | Elevated with prolonged aggressive fasting | Moderate risk |
| Thyroid (T3) | ↓ up to 55% during 24-hour fasts | Fully reversible upon refeeding | Low risk with short fasts; monitor with extended |
| BDNF | ↑ | Neuroprotective | High benefit |
Sources: PMC12330278, PMC9182756, PMC9877115.

Estrogen And Progesterone: What Short-Term TRE Actually Does
The good news: an 8-week controlled study of 23 women on a 4–6 hour eating window found that estradiol, estrone, and progesterone remained essentially unchanged. Short-term time-restricted eating, producing 3–4% body weight reduction, has little effect on sex steroid levels in most women.
DHEA decreased by 13–14% in both premenopausal and postmenopausal groups. DHEA is a precursor to both estrogen and testosterone. Those levels stayed within normal ranges in this study, but the long-term implications of sustained DHEA reduction deserve monitoring — particularly in women over 40.
The real risk to female reproductive hormones isn't moderate TRE. It's aggressive, calorie-restricted fasting. GnRH — the hormone that initiates the entire estrogen-progesterone cascade — is sensitive to energy deficit and physiological stress. When fasting tips from managed restriction into a significant caloric deficit, GnRH secretion can be suppressed, disrupting the menstrual cycle. If your periods become irregular after starting IF, the fasting is a likely cause, and the protocol needs adjustment immediately.
For a broader look at how the female metabolism responds to dietary changes, see Understanding the Female Metabolism.
Testosterone And Androgens: The PCOS Evidence
A 2022 review of three human trials found that intermittent fasting significantly decreases androgen markers in premenopausal women and those with PCOS, with the strongest effects when calories are consumed earlier in the day:
- Li et al. (n=18, 5 weeks): 9% decrease in total testosterone, 26% decrease in Free Androgen Index (FAI)
- Jakubowicz et al. (n=60, 12 weeks): 50% decrease in free testosterone when more than 50% of calories were consumed at breakfast vs. dinner
- Harvie et al. (n=107, 24 weeks): 6–10% decrease in FAI
Sex hormone binding globulin (SHBG) increased by 2–14% across all three studies. SHBG binds free testosterone, reducing its activity — which is directly therapeutic for the symptoms of androgen excess in PCOS.
The authors are clear about limitations: sample sizes are small, study durations short, and strong conclusions aren't yet warranted. But the direction of the evidence is consistent and meaningful for women managing PCOS.
Cortisol: The Hidden Risk
Cortisol is the most underreported hormone story in women's IF research. According to the 2024 PMC review on hormonal regulation:
- Extended fasting (72 hours) significantly elevated cortisol, ACTH, adrenaline, and noradrenaline
- Time-restricted eating without caloric restriction lowered cortisol
- Isocaloric TRE (same calories, just restricted timing) raised cortisol
- Older women experience greater cortisol increases from fasting than younger women
Chronically elevated cortisol drives abdominal fat accumulation, disrupts sleep, suppresses immune function, and — critically — can blunt the fat-burning effects you're fasting to achieve. If you're fasting hard and gaining belly fat, cortisol is the first place to look. The full cortisol-belly fat connection is covered here.
The practical rule: fasting without meaningful caloric restriction (i.e., eating normally within your window) lowers cortisol. Fasting on top of an already large caloric deficit pushes cortisol up. This is why undereating in the eating window is counterproductive, not just for hormones but for results.
Thyroid Hormones
A 24-hour fast can decrease serum T3 by up to 55% with no change in TSH — this is a metabolic conservation mechanism, not thyroid disease, and it reverses fully upon refeeding. Occasional extended fasts likely don't affect thyroid function long-term.
But if you're doing frequent 24-hour fasts and noticing fatigue, cold sensitivity, hair thinning, or constipation, the thyroid suppression pattern is worth discussing with your doctor. The keyword is frequent — once-monthly 24-hour fasts in healthy women are a different category from weekly extended fasting.

Cycle-Syncing Your Intermittent Fasting Window
This is the piece most IF guides don't include — and the reason many women give up on fasting that could actually work for them.
Your menstrual cycle creates real, measurable shifts in caloric needs, insulin sensitivity, and stress hormone tolerance. Applying a fixed 16-hour window every day, regardless of cycle phase, is the dietary equivalent of training at maximum intensity every day, regardless of recovery. The protocol that works in the follicular phase actively works against you in the late luteal phase.
Cycle-syncing your fasting window means adjusting fasting length and meal timing based on where you are in your cycle. You're still getting the benefits of IF — just matched to your biology.
See the companion article on cycle syncing for weight loss for the full nutrition and workout approach.
Days 1–10: Follicular Phase — Your Fasting Sweet Spot
Estrogen is rising and insulin sensitivity is higher than at any other phase. Energy tends to be good. This is when 16–18 hour fasting windows are best tolerated and most metabolically effective.
If you want to experiment with a longer window or an occasional 24-hour fast, the follicular phase is where to do it. Fat burning is more accessible, cortisol response is lower, and the hormonal environment is most forgiving. Push here.
Days 11–15: Ovulatory Phase — Slight Adjustment
Estrogen peaks and then LH surges to trigger ovulation. Energy is high, but many women notice a spike in hunger around ovulation. A 14–16 hour window is appropriate. Fighting intense mid-cycle hunger with a full 18-hour window is one of those places where the rigid approach raises cortisol more than it burns fat. Ease off by 1–2 hours.
Days 16–24: Luteal Phase — Ease Up
Progesterone rises sharply after ovulation. This hormone elevates basal metabolic rate by an estimated 100–300 calories per day — and raises appetite to match. Insulin sensitivity drops compared to the follicular phase.
Aggressive fasting in the luteal phase is where women most commonly run into trouble. Cortisol climbs more easily. Hunger is more intense and more biologically legitimate. The energy deficit created by a 16-hour fast on top of elevated progesterone-driven metabolic needs can suppress GnRH and trigger the hormonal disruption discussed earlier.
A 12–14 hour fasting window during this phase is the right balance — roughly the overnight fast that most people do naturally. You're still capturing metabolic benefits without fighting your own hormones.
Fasting Burns Fat Faster
"Periodic fasting can help clear up the mind and strengthen the body and the spirit." - Ezra Taft Benson.
Days 25–28: Late Luteal / Premenstrual Phase — Trust Your Signals
If you're exhausted, experiencing significant PMS symptoms, or your hunger is noticeably higher than usual, breaking the fast earlier is not a failure. The physiological stress of forcing a fast you're not recovering from outweighs the benefit.
A 12-hour window — stop eating at 8 pm, eat again at 8 am — is entirely sufficient. The goal during this phase is to preserve the habit without adding hormonal stress.
The Women's Fasting Framework
Most IF protocols give you a rule. This framework gives you a system. The Women's Fasting Framework adjusts three variables across the menstrual cycle:
- Window length — how many hours you fast
- Meal timing — whether you front-load or back-load calories within the eating window
- Recovery flexibility — permission to modify on high-stress, premenstrual, or low-energy days
| Cycle Phase | Window Length | Meal Timing | Flexibility Rule |
|---|---|---|---|
| Follicular (Days 1–10) | 16–18 hours | Standard (noon–8pm) | Extend if energy supports it |
| Ovulatory (Days 11–15) | 14–16 hours | Front-load when possible | Adjust by hunger |
| Luteal (Days 16–24) | 12–14 hours | Front-load (larger meals before 3pm) | Shorten if cortisol signs appear |
| Premenstrual (Days 25–28) | 12 hours or less | Flexible | Break earlier if needed — no penalty |
On front-loading: Research shows that consuming more than 50% of daily calories earlier in the day produces significantly better androgen reduction in PCOS and meaningfully improves insulin sensitivity compared to evening-weighted eating patterns. This applies regardless of fasting window length — and it's a lever many women never adjust.
Who Should Not Do Intermittent Fasting
Do not practice intermittent fasting if you:
- Are under 18 years old
- Are you pregnant or breastfeeding
- Have Type 1 diabetes or are insulin-dependent
- Have a current or past history of an eating disorder (anorexia, bulimia, binge eating disorder, ARFID)
- Are you experiencing amenorrhea (loss of menstrual cycle) unrelated to menopause
- Are currently underweight (BMI below 18.5)
- Take medication that requires food at specific intervals
If you are perimenopausal or postmenopausal, have thyroid or adrenal conditions, or have been diagnosed with PCOS, IF can still be appropriate — but start with a shorter window and discuss it with your healthcare provider first. For perimenopausal-specific strategies, see How to Lose Weight During Perimenopause Without Starving Yourself.
Join Our Mailing List
Join thousands of women inside our community and receive our free guide, 10 Actions That Support Permanent Weight Loss — the exact behavioural shifts that make the difference between a two-week attempt and a lasting transformation.
No restriction plans. No guilt. Just what actually works — for real women with real lives.

Common Mistakes Women Make With Intermittent Fasting
Starting Too Aggressively
Going from no fasting to a strict 16-hour window on day one is a setup for the cortisol spike, hunger misery, and abandonment by week two that gives IF a bad reputation. Start with 12 hours — which most people are already doing overnight — and extend by 30 minutes each week. Your results will not be slower. They'll be better because you'll actually sustain it.
Undereating During The Eating Window
IF is not a license for drastic caloric restriction. If you're eating 1,000 calories in an 8-hour window when your body needs 1,800, you're in a significant deficit — and your hormonal axis will respond accordingly. Focus on protein-first eating during your eating window. Aim for 0.7–1g of protein per pound of lean body mass. This is the single biggest factor in preserving muscle mass while fasting.
Treating Every Day As Identical
Rigid daily fasting without adjusting for cycle phase, sleep quality, or stress load is how women burn out on IF within 6–8 weeks. The Women's Fasting Framework adjusts for this. Inflexible protocols don't.
Neglecting Sleep Quality
Your fasting window is mostly overnight, which means sleep directly affects your fasting outcomes. Poor sleep raises ghrelin the next morning and reduces insulin sensitivity, both undercutting the work the overnight fast is doing. Sleep and weight loss in women are more tightly linked than most people realize — treat sleep as part of the fasting strategy.
Breaking The Fast With Ultra-Processed Foods
What you eat in your eating window determines whether IF is a metabolic health strategy or just restricted-window calorie consumption. Breaking your fast with high-sugar foods spikes insulin sharply and negates much of the insulin-sensitivity benefit the fasting period produced. Break your fast with protein and healthy fats — eggs, Greek yogurt, avocado, or a high-protein smoothie.
For specific morning meal guidance, see What Should Women Eat in the Morning for Hormone Balance and Fat Loss.
What To Eat During Your Intermittent Fasting Window
Protein comes first. Aim for 0.7–1g per pound of lean body mass, spread across your eating window. Protein preserves muscle during periods of caloric restriction, supports satiety through the fasting hours, and has a higher thermic effect than carbohydrates or fat. If you consistently undereat protein while fasting, muscle loss is the predictable result.
Healthy fats — avocado, olive oil, nuts, fatty fish — blunt insulin response after meals and extend satiety. They also support estrogen production, which matters given the hormonal context of this guide.
Fiber-rich carbohydrates — vegetables, legumes, whole grains — slow digestion, feed beneficial gut bacteria, and support blood sugar stability. The gut-hormone axis is real: microbiome disruption correlates with hormonal dysregulation in multiple studies.
What breaks a fast: Technically, any caloric intake. Practically, black coffee and plain tea do not meaningfully interrupt the metabolic state of fasting. Water is always fine. Adding cream, sugar, or any food ends the fast. For the purposes of most health goals, some flexibility here is fine — consistency over the long run matters more than perfection on any given day.
For a complete approach to eating for sustainable results, see Weight Loss Without Counting Calories and the Ultimate Guide to Sustainable Fat Loss.
The companion guide on intermittent fasting specifically for fat loss goes deeper into the body composition side. The sustainable fat loss guide covers the broader context. Put them together, and you have a complete framework — not another diet that stops working after six weeks.
Related Articles
The Bottom Line
Intermittent fasting works for women — but not by following the same playbook as men, and not by applying a rigid protocol regardless of where you are in your hormonal cycle.
The evidence is genuinely strong on insulin sensitivity and PCOS-related androgens. The autophagy science is real. The brain benefits are biologically grounded. What the research also shows clearly is that fasting too aggressively, too rigidly, or in the wrong cycle phase raises cortisol, can suppress reproductive hormones, and produces the exact opposite of the results women are fasting for.
The Women's Fasting Framework covered in this guide — adjusting window length and meal timing by cycle phase, front-loading calories, starting conservatively — closes that gap. It's not a softer version of IF. It's a version calibrated to how women's metabolism actually works.
Glossary Of Key Terms
FAQ
Intermittent fasting can cause muscle loss — but it doesn't have to. The primary driver is insufficient protein intake, not the fasting itself. Studies show that time-restricted eating combined with adequate protein (0.7–1g per pound of lean mass) and resistance training preserves lean mass effectively. If you're fasting without either, muscle loss is a real risk.
Strength training for women over 40 covers the resistance training side of this equation.
Yes, with adjustments. Low-to-moderate cardio works well in the fasted state and may enhance fat oxidation. Heavy strength training fully fasted is harder — most women notice performance decrements, and muscle protein synthesis needs available amino acids. A practical approach: schedule workouts near the end of your fasting window, then break your fast immediately after. This captures the metabolic benefits of fasted training while supporting recovery with protein.
Most women notice changes in energy levels and hunger patterns within 1–2 weeks. Visible body composition changes typically appear at 4–8 weeks of consistency. The deeper metabolic adaptations — improved insulin sensitivity, more efficient fat oxidation — continue developing over months. Expecting dramatic results in two weeks and quitting when they don't appear is the most common reason IF "doesn't work."
It can, because perimenopausal weight gain is strongly linked to insulin resistance, and IF has documented effects on insulin sensitivity at multiple timescales. The best dietary approaches for women over 40 include IF as one tool among several. It works better when combined with adequate protein, resistance training, and attention to cortisol management.
Postmenopausal women should note that the cortisol response to fasting is greater in older women — shorter windows (12–14 hours) may be the better starting point than jumping to 16/8.
They're not the same thing, though they often overlap. A calorie deficit means eating fewer calories than you burn. Intermittent fasting is a timing restriction that may or may not create a caloric deficit, depending on what you eat in your eating window.
The metabolic benefits of IF — autophagy, insulin sensitivity improvement, and BDNF increase — are partly independent of caloric restriction. You can get them even if they are eating the same total calories, just compressed into a shorter window. That said, many people naturally eat less when they limit their eating window, which creates an unintentional caloric deficit that drives additional fat loss.
Some women find that structured eating windows reduce the opportunity for mindless or stress-driven eating. That can help — but it's structural, not psychological. For the emotional eating side, there's a different toolkit. How mindfulness can break the cycle of emotional eating is worth reading alongside any fasting protocol, and the connection between diet and stress-related weight gain in women is covered in more depth separately.
Intermittent fasting is an eating pattern that cycles between defined periods of fasting and eating. It does not restrict what you eat — only when. The most common method is the 16/8 protocol: 16 hours fasting, 8 hours eating each day.
After 12 hours without food, the body depletes glycogen stores and shifts from burning glucose to burning stored fat — the metabolic switch. This produces ketones and triggers autophagy, the cellular repair process that won Yoshinori Ohsumi the 2016 Nobel Prize in Medicine.
Short-term time-restricted eating (16/8) is generally safe for healthy premenopausal women. It is not appropriate for those who are pregnant, nursing, diabetic, underweight, or have eating disorder history. Aggressive fasting can disrupt cortisol, GnRH, and thyroid function in women already under metabolic stress.
You Know Why. Now Learn Exactly How
Join thousands of women inside our community and receive our free guide: 10 Actions That Support Permanent Weight Loss — the practical, sustainable habits that translate everything you just read into real, lasting results.
No fad diets. No extreme plans. Just what the research actually supports — written for real women.

