How To Lose Weight During Perimenopause Without Restrictive Dieting
Eleanor Roosevelt
Strength Under Pressure
A woman is like a tea bag — you never know how strong she is until she gets into hot water.
The Executive Summary
During perimenopause, hormonal shifts impact fat storage, muscle building, and blood sugar. Weight loss requires a different approach than simple calorie restriction. A high-protein, anti-inflammatory diet combined with resistance training is effective for fat loss and muscle preservation.
Prioritize sleep to manage cortisol and insulin levels. Intermittent fasting with a 12–14-hour overnight fast may be beneficial. Focus on muscle mass by consuming 0.7–1.0g of protein per pound of body weight daily to counteract muscle loss.
Somewhere between 40 and 50, many women notice that the approach that always worked — eat a little less, move a little more — stops delivering results. Clothes that fit last spring don't. Sleep deteriorates. Energy dips. And the scale drifts upward despite nothing obviously changing.
This is perimenopause: the years-long hormonal transition that precedes menopause, typically beginning in the early-to-mid 40s. It is not a personal failure, a metabolism mystery, or an inevitable price of getting older. It is a measurable shift in hormonal environment — one that changes how your body stores fat, builds muscle, manages blood sugar, and responds to stress.
Understanding those changes makes them workable. You do not need to eat less. You need to eat differently. You do not need to exercise harder. You need to exercise smarter. And you do not need to starve yourself — a strategy that, in perimenopause, tends to make things considerably worse.
This guide covers what changes during perimenopause and the specific diet, exercise, sleep, and supplement strategies that work with your shifting biology instead of fighting it.
Medical & Referral Disclaimer
This article is for informational and educational purposes only. It is not a substitute for professional medical advice, diagnosis, or treatment. Always consult your physician or qualified health provider before starting any new diet or exercise program.
Key Takeaways
- Perimenopause weight gain — especially belly fat — is driven by hormonal shifts in estrogen, cortisol, and insulin, not aging or overeating alone.
- Cutting calories aggressively often backfires: chronic restriction raises cortisol, accelerates muscle loss, and deepens hormonal imbalance — the opposite of what perimenopausal women need.
- A high-protein, anti-inflammatory diet paired with resistance training is the most evidence-backed combination for fat loss and muscle preservation after 40.
- Sleep quality is a metabolic lever: poor sleep raises ghrelin, cortisol, and insulin resistance — all of which directly promote visceral fat storage.
- Intermittent fasting can work for some women, but aggressive protocols often worsen hormonal symptoms; a 12–14-hour overnight fast is the safer starting point.
- HRT does not cause weight gain and may actively reduce visceral fat — consult your physician for a personalized assessment based on current evidence.
How Much Protein Do Perimenopausal Women Actually Need?
Perimenopausal women need significantly more protein than standard guidelines suggest — approximately 0.7–1.0g per pound of body weight (1.6–2.2g per kg) per day. This elevated target counteracts accelerated muscle loss, preserves metabolic rate, reduces hunger hormones, and supports bone density during the menopause transition.
Most women in midlife eat 40–60g of protein daily. Reaching 100–130g is one of the highest-leverage changes a perimenopausal woman can make.
Protein And Muscle Preservation After 40
Every pound of muscle burns approximately 6 calories at rest. During perimenopause, muscle loss accelerates due to declining estrogen and lower anabolic hormone levels. Without deliberate protein intake and resistance training, this loss compounds year on year — lowering metabolic rate progressively.
Research consistently shows that protein intakes of 1.6g/kg or higher preserve significantly more lean mass during caloric deficits than lower intakes. This is not optional for perimenopausal women trying to manage weight — it is foundational.
For preparation strategies and protein-per-serving data, see our guide to 5 Powerful Protein Foods for Dieting.
Best Lean Protein Sources For Midlife Women
- Greek yogurt (plain) — 17g per 170g serving; also delivers calcium and probiotics.
- Salmon — 22g per 85g serving; omega-3s additionally support inflammation and hormonal health.
- Chicken breast — 31g per 100g; versatile and budget-friendly.
- Eggs — 6g each; whole eggs provide choline, critical for liver function and hormonal clearance.
- Firm tofu — 8g per 100g; phytoestrogen content is an additional benefit.
- Cottage cheese — 11g per 100g; slow-digesting casein is ideal before bed for overnight muscle repair.
- Lentils — 9g per 100g cooked, plus 16g fiber per serving.
For morning protein strategies, see what women should eat in the morning for hormone balance and fat loss.

Does Intermittent Fasting Work For Perimenopause Weight Loss?
Intermittent fasting can support weight loss during perimenopause, but aggressive protocols — 20:4 windows or extended daily fasts — often increase cortisol, worsen sleep disruption, and exacerbate hormonal imbalance in women already in a hormonally stressed state. A 12–14-hour overnight fast is the safer, evidence-supported starting point.
The popular advice to simply "skip breakfast" is not appropriate for all perimenopausal women.
The Case For and Against IF In Perimenopause
Potential benefits:
- Improves insulin sensitivity — directly relevant to perimenopausal fat accumulation.
- May reduce inflammatory markers.
- Supports cellular cleanup (autophagy) during fasting periods.
- Simplifies food decisions, reducing total intake for some women.
Potential risks:
- Extended fasts spike cortisol — the same hormone driving visceral belly fat.
- Skipping breakfast can worsen blood sugar volatility in insulin-resistant women.
- Fasting-induced stress worsens sleep disruption, hot flashes, and mood instability in some women.
- May accelerate muscle loss if protein targets aren't met within shorter eating windows.
A Gentler Approach — Time-Restricted Eating For Perimenopausal Women
A 12–14-hour overnight fast (for example: finish dinner by 7 pm, eat breakfast by 7–9 am) captures the metabolic benefits without the cortisol elevation of longer windows.
This approach:
- Supports overnight insulin reset.
- Allows protein to be distributed across 3 full meals.
- Doesn't require skipping breakfast (which maintains stable morning cortisol).
- Is sustainable as a permanent eating pattern.
Our Ultimate Guide to Intermittent Fasting covers protocols in detail, including which approaches suit different goals and metabolic profiles.

What Exercise Works Best For Losing Weight During Perimenopause?
The best exercise combination for perimenopause weight loss is resistance training 2–3 times per week paired with low-intensity daily movement such as walking, yoga, or swimming. This combination preserves muscle mass, supports bone density, improves insulin sensitivity, and avoids the cortisol spike that high-intensity cardio-only training produces in hormonally stressed women.
The longstanding prescription of daily cardio is particularly problematic in perimenopause, where excess cortisol is already a primary driver of belly fat.
Why Resistance Training Is The Priority After 40
Resistance training — weights, bands, or progressive bodyweight exercises — is the most potent single intervention for reversing the metabolic and muscular decline of perimenopause.
Benefits specific to perimenopausal women:
- Directly counters estrogen-driven muscle loss.
- Raises basal metabolic rate (more muscle = more calories burned at rest).
- Improves insulin sensitivity for 24–48 hours post-session.
- Strengthens bones — critical as estrogen decline increases fracture risk.
- Stimulates growth hormone, which supports fat metabolism and muscle repair.
- Has been shown in randomized trials to reduce hot flash frequency in some women.
Start with 2 sessions per week, 30–45 minutes each. Progressive overload — gradually increasing resistance or difficulty over time — is what produces long-term results. For a structured beginner plan, see fat loss workouts for beginners.

Why High-Volume Cardio Can Backfire In Perimenopause
Running five days a week or attending daily high-intensity classes chronically elevates cortisol — particularly harmful when cortisol is already raised by hormonal disruption, disrupted sleep, and life stress.
This does not mean cardio is harmful. Low-intensity movement — walking, swimming, cycling at a conversational pace — reduces stress hormones rather than raising them. Yoga directly activates the parasympathetic nervous system, lowering cortisol measurably.
Evidence-based weekly structure for perimenopausal fat loss:
- 2–3x resistance training (30–45 minutes)
- 3–5x low-intensity walking (20–45 minutes)
- 1–2x yoga or restorative movement
- 0–1x moderate-intensity cardio (swimming, cycling)
Why Walking Deserves More Credit Than It Gets
A daily 30-minute walk is not a consolation prize. Research published in the British Journal of Sports Medicine shows that regular walking significantly reduces visceral fat, improves insulin sensitivity, and lowers cortisol — addressing three of the four primary drivers of perimenopausal weight gain simultaneously. It is also low-impact, sustainable, and requires no gym membership.

How Does Sleep Affect Weight During Perimenopause?
Poor sleep directly causes weight gain during perimenopause by raising ghrelin (the hunger hormone), reducing leptin (the satiety hormone), elevating cortisol, and worsening insulin resistance — all of which promote fat storage, particularly in the abdomen. Women who sleep fewer than 7 hours per night consistently show higher rates of visceral fat accumulation, independent of diet and exercise.
Sleep disruption is among the most common and most underaddressed perimenopause symptoms — and one of the highest-leverage variables to address for fat loss.
The Sleep-Cortisol-Fat Storage Loop
Poor sleep → cortisol rises → insulin resistance worsens → more abdominal fat stored → inflammatory visceral fat disrupts sleep → poor sleep. This cycle is self-reinforcing. Breaking it requires addressing sleep quality directly, not just diet and exercise.
Night sweats and hot flashes fragment sleep architecture. Even when total sleep time appears adequate, disrupted sleep stages reduce growth hormone secretion — which is critical for overnight fat metabolism — and impair the cortisol reset that healthy sleep provides.
Practical Sleep Hygiene Strategies For Perimenopausal Women
- Keep the bedroom cool (65–68°F / 18–20°C) — directly reduces night sweat frequency and severity.
- Limit alcohol — even one drink disrupts sleep architecture and triggers hot flashes in many women.
- Magnesium glycinate (300–400mg before bed) — supports GABA production, promotes deeper sleep stages, reduces nighttime cortisol.
- Consistent sleep and wake times — regulates circadian cortisol rhythm.
- Reduce blue light 90 minutes before bed — supports melatonin production, which declines with age.
- Evening protein snack (cottage cheese or Greek yogurt) — stabilizes overnight blood sugar, reducing early-morning cortisol spikes.
If fatigue persists beyond sleep quality issues, there may be underlying factors worth discussing with your physician — our guide on why you feel tired all the time covers common contributors.
Should Women Consider HRT For Perimenopause Weight Management?
HRT (hormone replacement therapy) does not cause weight gain and, for many women, actively reduces visceral fat accumulation by restoring estrogen's role in fat distribution and insulin sensitivity. Current evidence — including updated guidance from the North American Menopause Society — supports HRT as safe and appropriate for most healthy women under 60 who begin within 10 years of menopause onset.
This is a medical decision between you and your physician — but it should be based on current evidence, not the outdated fears generated by the 2002 WHI study, which has since been substantially reanalyzed.
What The Research Actually Shows About HRT And Weight
Updated meta-analyses consistently show:
- HRT does not increase total body weight.
- Estrogen therapy reduces central (visceral) fat accumulation compared to placebo.
- Women on HRT preserve more lean muscle during the menopause transition.
- Improved sleep from hot flash reduction indirectly supports weight regulation.
- Transdermal estrogen (patches, gels) carries a lower risk profile than oral forms.
Natural Hormone Support Strategies
For women not pursuing HRT, or using it alongside lifestyle strategies:
- Phytoestrogen-rich foods (flaxseed, soy, legumes) — provide mild estrogenic activity.
- Adaptogenic herbs (ashwagandha, rhodiola) — moderate evidence supports cortisol regulation.
- Reducing xenoestrogen exposure — minimize BPA plastics, pesticide-heavy produce, and certain synthetic fragrances that disrupt the endocrine system.
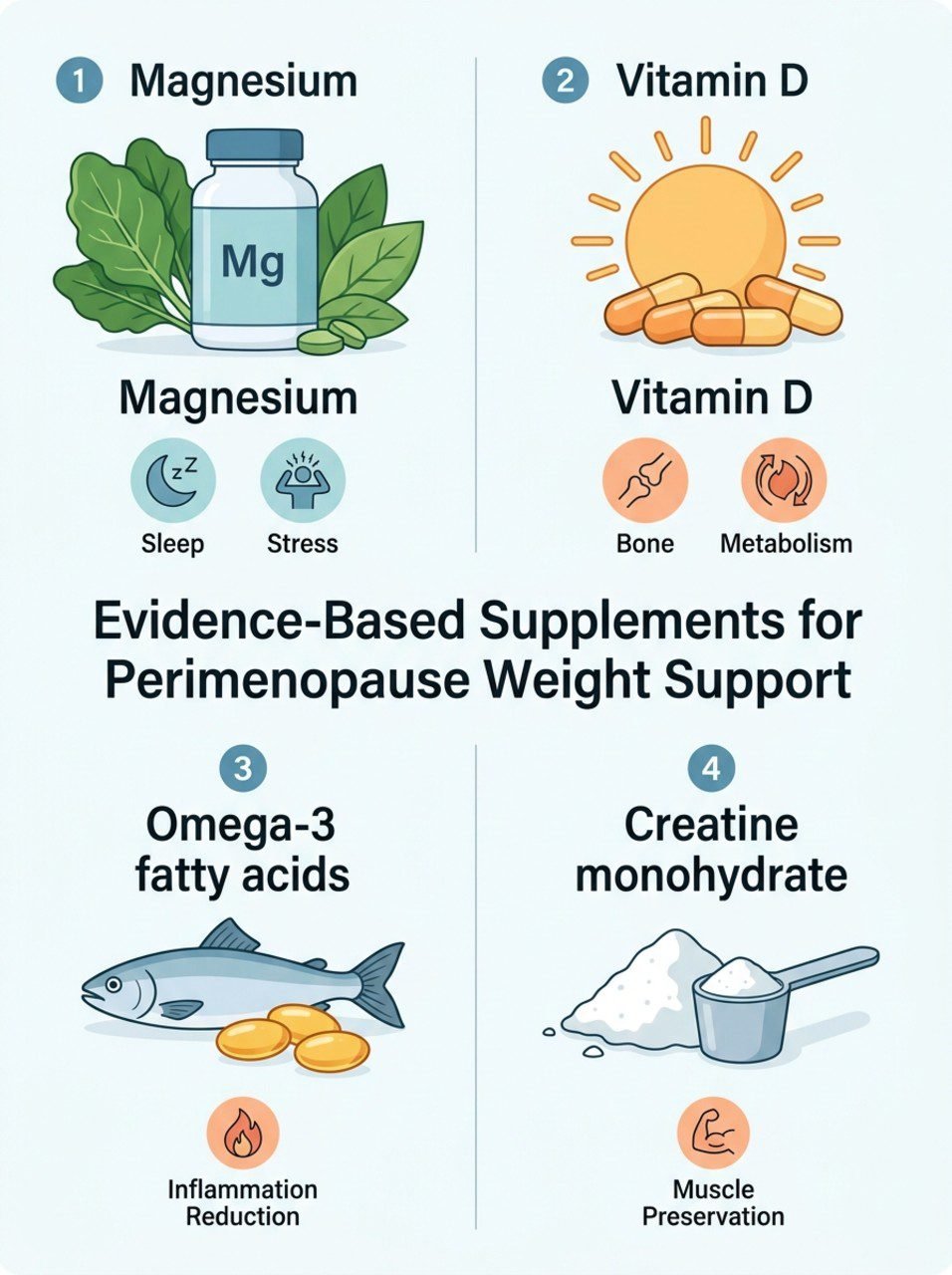
What Supplements Have the Strongest Evidence For Perimenopause Weight Support?
The supplements with the strongest evidence for perimenopause weight support are magnesium, vitamin D, omega-3 fatty acids, and creatine monohydrate. These address specific deficiencies and metabolic challenges common in perimenopausal women — rather than promising direct fat burning.
Supplements are support, not solutions. No supplement replaces protein intake, resistance training, sleep quality, or a whole-food diet.
Magnesium — The Most Important Perimenopause Mineral
Magnesium is involved in over 300 enzymatic reactions, including cortisol regulation, insulin sensitivity, thyroid function, and sleep. Perimenopausal women are disproportionately deficient: estrogen decline reduces magnesium retention, and chronic stress depletes it further.
- Dose: 300–400mg magnesium glycinate or malate daily (glycinate for sleep; malate for energy and muscle function).
- Food sources: Pumpkin seeds, spinach, almonds, black beans, dark chocolate.
Evidence-Based Supplement Stack For Perimenopause
| Supplement | Primary Benefit | Dose | Notes |
|---|---|---|---|
| Magnesium glycinate | Cortisol, sleep, insulin sensitivity | 300–400mg at night | Most deficient mineral in perimenopausal women |
| Vitamin D3 + K2 | Insulin sensitivity, mood, bone density | 2,000–4,000 IU D3 daily | Take with K2 for synergistic bone benefit |
| Omega-3 (EPA+DHA) | Inflammation, cortisol, visceral fat | 2–3g EPA+DHA daily | Fish oil or algae oil |
| Creatine monohydrate | Muscle preservation, cognitive function | 3–5g daily | Underused in women; strong evidence base |
| Ashwagandha (KSM-66) | Cortisol reduction, stress resilience | 300–600mg daily | Allow 8–12 weeks to assess effect |
See our PDF guide to fat loss supplements for faster results, for complete evidence levels and what to avoid.
Related Articles
The Bottom Line
Perimenopause is a transition, not a dead end.
The weight changes that come with it are real and hormonally driven — but they are not permanent, and they are not beyond your influence. The approach that stopped working isn't failing because you failed. It's failing because the biological environment changed, and the strategy needs to change with it.
You don't need to eat less. You need more protein, more fiber, more resistance training, and more sleep. You need to manage cortisol — which means less aggressive dieting and less exhausting cardio, not more.
Start with one change. Add a protein source to breakfast tomorrow. Block two resistance training sessions into your week. Go to bed 30 minutes earlier. Any one of these, done consistently, shifts the trajectory.
Embrace Inspiration
Like What You Read? Be Sociable, Comment, And Share It! Thanks.
Glossary Of Key Terms
FAQ
Declining estrogen shifts fat storage from the hips and thighs to the abdomen — this is a hormonal change, not a lifestyle failure. To address it specifically, reduce insulin spikes through lower refined carbs and more fiber and protein, manage cortisol through sleep and stress reduction, and add progressive resistance training.
In most cases, no. Severe restriction raises cortisol, accelerates muscle loss, and deepens hormonal imbalance — making long-term fat loss harder, not easier. A moderate deficit of 200–400 calories below maintenance, paired with high protein and resistance training, produces better sustainable results. Use our calorie calculator to find your baseline.
The hormonal shifts are real, but significant weight gain is not inevitable. Women who maintain resistance training, adequate protein, quality sleep, and stress management consistently show much smaller changes in body composition during the perimenopause transition than those who don't address these factors.
Perimenopause typically lasts 4–10 years, beginning in the early-to-mid 40s for most women. Hormonal fluctuations are irregular throughout this period, which is why symptoms and weight management difficulty can vary significantly week to week.
Yes, and disproportionately. Alcohol elevates estrogen, worsens insulin resistance, disrupts sleep architecture, and contributes 7 calories per gram with no nutritional value. Even moderate alcohol consumption measurably worsens hot flashes, night sweats, and abdominal fat accumulation in perimenopausal women.
Start resistance training. No other intervention addresses as many of perimenopause's fat-driving mechanisms at once: it preserves muscle, raises metabolic rate, improves insulin sensitivity for 24–48 hours, strengthens bone, and reduces hot flash frequency in some women.
You Know Why. Now Learn Exactly How
Join thousands of women inside our community and receive our free guide: 10 Actions That Support Permanent Weight Loss — the practical, sustainable habits that translate everything you just read into real, lasting results.
No fad diets. No extreme plans. Just what the research actually supports — written for real women.
