The Science Behind Depression-Related Weight Gain in Women, and the Compassionate, Practical Path Forward
John Green
There Is Always Hope
There is hope, even when your brain tells you there isn't.
The Executive Summary
The connection between depression and weight gain in women is well-documented, stemming from hormonal, neurochemical, and metabolic changes. Elevated cortisol promotes abdominal fat storage and cravings, while reduced motivation impacts physical activity.
Antidepressants and nutritional deficiencies can also contribute. Addressing both mental and physical health through small, sustainable steps is crucial. This is a biological response, not a personal failing, requiring compassionate strategies for change.
You've noticed the weight creeping up. You know you haven't been eating perfectly. You know you haven't been moving much. And if you're living with depression, there's a good chance you've layered guilt on top of all of it — telling yourself you just need more willpower, more discipline, more effort.
I want to offer you something different. This is not a character flaw. This is biology.
The connection between depression and weight gain is one of the most documented — and least discussed — relationships in women's health. It isn't simply about comfort eating, though that's part of it. It runs through your hormones, your brain chemistry, your sleep architecture, your medications, and the specific nutritional depletions that depression creates.
Understanding why this happens is not an excuse. It is the starting point for doing something about it — with compassion, not punishment.
Medical & Referral Disclaimer
This article is for informational and educational purposes only. It is not a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or a qualified mental health professional regarding any questions about depression, medication, or treatment. If you are in crisis, please contact a mental health helpline in your country immediately.
Key Takeaways
- Depression-related weight gain is a biological process, not a failure of willpower.
- Chronic cortisol elevation directly promotes abdominal fat storage and high-calorie food cravings.
- Reduced physical activity in depression is a neurobiological symptom — not laziness.
- SSRIs and some other antidepressants can cause weight gain as a documented side effect — always discuss this with your doctor before making any changes.
- Depression depletes omega-3 fatty acids, B vitamins, vitamin D, and zinc — all of which affect metabolism and mood.
- Sleep disruption caused by depression raises hunger hormones and promotes fat storage.
- Breaking the cycle requires addressing both mental and physical health simultaneously — small, sustainable steps compound over time.
Can Depression Really Make You Gain Weight?
Yes — depression causes weight gain through multiple biological mechanisms, including elevated cortisol, reduced physical activity, disrupted sleep, nutritional deficiencies, and medication side effects. These are documented physiological processes, not personal failings.
The World Health Organization estimates that over 280 million people worldwide live with depression, and women are approximately twice as likely as men to be diagnosed with it. Among the most commonly reported physical effects is unexplained weight gain.
What makes this topic particularly important for women is that the biological drivers of depression-related weight gain interact with the hormonal realities of the female body in ways that aren't well understood by most generic health advice.
The result: women struggling with depression often receive guidance on weight management that completely ignores the underlying physiology, making their situation different. This article corrects that.
Reason #1: Depression can deplete motivation, but this is not the same as being lazy
Depression fundamentally reduces the neurological capacity for motivation and energy, making physical activity feel genuinely unattainable — not through lack of effort, but through disrupted dopamine and serotonin pathways that govern drive, reward, and the will to act.
How Does Depression Affect Physical Activity Levels In Women?
When you're well, deciding to exercise is relatively simple. Your brain's reward system fires in anticipation — you feel a pull toward the activity and a burst of satisfaction when you complete it. That system runs on dopamine.
Depression disrupts dopamine regulation. The anticipatory reward signal is blunted. The effort required feels enormous. The payoff feels remote. This is not a mindset problem — it is a documented neurobiological feature of depressive disorders.
The practical consequence: physical inactivity. And physical inactivity has a direct relationship with weight gain — through reduced calorie expenditure, muscle loss, slower metabolism, and worsening insulin sensitivity.
This creates one of depression's most vicious cycles:
- Depression reduces motivation to exercise
- Physical inactivity contributes to weight gain
- Weight gain worsens body image and low mood
- Worsened mood deepens depression
- Deeper depression further reduces motivation
Understanding that step one is neurobiological — not moral — is crucial to breaking this cycle without self-blame.
What Can You Do When Depression Makes Exercise Feel Impossible?
The key insight here: you don't need a full workout. You need a signal.
Research published in JAMA Psychiatry found that even 15 minutes of vigorous activity or one hour of walking per week was associated with a 26% reduction in depression risk. The threshold for benefit is dramatically lower than most exercise guidance suggests.
Entry-level strategies that respect where you actually are:
- A 5-minute walk outside — natural light alone has a measurable effect on serotonin.
- One set of 10 bodyweight squats — not for the calories, but for the neurological signal.
- Gentle yoga or stretching — reduces cortisol without requiring high motivation.
- Movement bundled with something enjoyable — a podcast, an audiobook, music that matters to you.
The goal at this stage is not fitness. It is interrupting the inactivity spiral with the minimum effective dose of movement.
When you're ready to build a fuller routine: Fat-Burning Workouts That Build Momentum →

Reason #2: Cortisol — The Depression-Stress Hormone That Drives Weight Gain
Chronic depression elevates cortisol — the body's primary stress hormone — to sustained high levels that directly promote abdominal fat storage, intensify cravings for calorie-dense foods, and impair the metabolic processes needed for healthy weight management.
What Does Chronic Cortisol Do to Your Body and Appetite?
In healthy amounts, cortisol is essential — it regulates metabolism, immune function, and the sleep-wake cycle. But cortisol was designed for short bursts of stress, not the sustained low-grade activation that characterises depression.
When cortisol stays elevated for weeks or months:
- Appetite increases — specifically for high-fat, high-sugar foods. This isn't a craving you can willpower your way through; it is a direct hormonal instruction.
- Insulin sensitivity decreases — your body processes carbohydrates less efficiently, leading to greater fat storage from the same food.
- Abdominal fat cells multiply — cortisol preferentially directs fat storage to the visceral (belly) region, which carries the greatest long-term health risk.
- Muscle tissue breaks down — cortisol is catabolic, meaning it breaks down muscle for energy, reducing the lean mass that keeps metabolism high.
- Serotonin is suppressed, perpetuating the very depression that is driving the cortisol elevation.
| Cortisol Effect | What It Causes in the Body | Result for Weight |
|---|---|---|
| Increased appetite signalling | Strong cravings for sugar, fat, and refined carbs | Higher daily calorie intake |
| Reduced insulin sensitivity | Poor blood sugar regulation | Greater fat storage from carbohydrates |
| Visceral fat promotion | Direct fat storage in the abdominal region | Belly fat accumulation |
| Muscle catabolism | Breakdown of lean muscle tissue | Lower resting metabolic rate |
| Sleep disruption | Reduced sleep quality and duration | Raised ghrelin (hunger hormone) |
| Serotonin suppression | Worsened mood and emotional eating | More comfort food seeking |
Why Does Depression Specifically Cause Belly Fat in Women?
Women carry a particular vulnerability here. Estrogen typically acts as a partial buffer against cortisol-driven abdominal fat storage — but during perimenopause and menopause, when estrogen declines, this protective effect diminishes.
Women in their late 30s and beyond experiencing depression may therefore see a pronounced increase in visceral fat during depressive episodes. Recognising cortisol-driven cravings as a physiological response rather than a character weakness is the first step toward managing them strategically.
For a deeper understanding of hormones and weight in women: How Hormones Affect Weight Loss in Women →
Reason #3: Some Antidepressants Contribute to Weight Gain
Certain antidepressant medications — particularly SSRIs and TCAs — list weight gain as a common documented side effect, placing some people in the genuinely difficult position of weighing essential mental health treatment against unwanted physical changes. This should always be discussed openly with your prescribing doctor.
Which Antidepressants Are Most Associated With Weight Gain?
It's important to note upfront: antidepressants save lives, and no one should stop taking prescribed medication without medical guidance. What follows is information to inform a conversation with your doctor — not a reason to discontinue treatment.
That said, weight gain is a documented side effect of several medication classes:
| Medication Class | Examples | Weight Gain Risk | Notes |
|---|---|---|---|
| SSRIs | Sertraline, Paroxetine, Citalopram | Moderate (varies by drug) | Paroxetine most commonly associated; Fluoxetine generally lower risk |
| TCAs (Tricyclic Antidepressants) | Amitriptyline, Nortriptyline | Higher | Older class; less commonly prescribed now |
| SNRIs | Venlafaxine, Duloxetine | Low to moderate | Generally lower risk than SSRIs |
| MAOIs | Phenelzine, Tranylcypromine | Higher | Rarely prescribed; significant dietary restrictions |
| Atypical antidepressants | Mirtazapine, Bupropion | Varies significantly | Mirtazapine higher risk; Bupropion is sometimes associated with weight loss |
Note: Individual response to medication varies significantly. This table reflects general trends in research, not guaranteed outcomes.
What Should You Do If You Suspect Your Medication Is Affecting Your Weight?
Talk to your doctor. This is not optional and not something to manage alone. Your prescribing physician can:
- Assess whether your weight change is likely medication-related or due to other factors.
- Discuss switching to a medication with a lower weight-gain profile, if appropriate for your condition.
- Adjust dosage in consultation with your clinical needs.
- Refer you to a registered dietitian for medication-specific nutritional guidance.
What you should not do is stop or reduce your antidepressants without medical supervision. Abrupt discontinuation carries serious risks. The goal is a managed conversation, not a unilateral decision.
Reason #4: Depression Depletes the Nutrients Your Metabolism Depends On
Depression is associated with documented deficiencies in several nutrients essential for metabolic function — including omega-3 fatty acids, B vitamins, vitamin D, and zinc — creating a physiological environment that promotes weight gain and impairs the body's capacity to respond to dietary changes.
Which Nutrients Are Most Depleted During Depression?
Research published in Nutritional Neuroscience and related journals has identified consistent patterns of nutritional deficiency in people with depression. These aren't incidental — they are part of a bidirectional relationship where nutritional status and mood directly affect each other.
Key nutrients depleted by depression:
- Omega-3 fatty acids — critical for brain function, inflammation regulation, and mood. Deficiency is associated with both worsened depression and impaired fat metabolism
- B vitamins (particularly B6, B9/folate, and B12) — essential for neurotransmitter synthesis (serotonin, dopamine) and efficient energy metabolism. Deficiency impairs the body's ability to convert food into usable energy
- Vitamin D — strongly associated with mood regulation; deficiency is more prevalent in people with depression, and is linked to disrupted metabolic function
- Zinc — required for thyroid function (which governs metabolic rate) and insulin regulation. Depression is associated with significantly lower zinc levels
- Magnesium — involved in over 300 enzymatic processes, including blood sugar regulation and stress hormone management
What Foods Help Break The Depression–Weight Gain Cycle?
| Nutrient | Best Food Sources | Effect on Depression-Related Weight |
|---|---|---|
| Omega-3 fatty acids | Salmon, mackerel, sardines, walnuts, flaxseeds | Reduces inflammation, improves mood, supports fat metabolism |
| Folate (B9) | Leafy greens, lentils, chickpeas, asparagus | Supports serotonin production; energy metabolism |
| Vitamin B12 | Eggs, dairy, meat, fortified plant milks | Essential for energy; deficiency causes fatigue and weight gain |
| Vitamin D | Oily fish, egg yolks, fortified foods, sunlight | Mood regulation; linked to metabolic health |
| Zinc | Red meat, pumpkin seeds, chickpeas, cashews | Thyroid function; insulin sensitivity |
| Magnesium | Dark leafy greens, nuts, seeds, dark chocolate | Stress hormone regulation; blood sugar balance |
A diet built around these nutrients does not need to be complex. A practical starting point: one palm-sized serving of oily fish twice a week, a daily handful of leafy greens, and eggs two to three times per week covers a significant portion of the most critical gaps.
For a practical approach to nutrition that supports both mood and weight: 3 Evidence-Based Tips for Women to Lose Weight →

The Fifth Factor: How Sleep Disruption and Inflammation Make Everything Worse
Sleep disruption — one of the most common symptoms of depression — independently raises the hunger hormone ghrelin by up to 15%, reduces the satiety hormone leptin, and triggers a low-grade inflammatory state that compounds cortisol dysregulation and further promotes fat storage.
How Does Poor Sleep From Depression Drive Weight Gain?
When depression disrupts sleep — through early waking, difficulty falling asleep, or non-restorative sleep — it directly alters the hormonal environment governing hunger and fat storage.
According to research from the University of Chicago, even two nights of short sleep (5.5 hours vs. 8.5 hours) increased ghrelin levels by 24% and reduced participants' ability to feel full from the same meal. For women experiencing chronic sleep disruption as part of depression, this hormonal shift is ongoing — meaning they are genuinely hungrier and less satisfied by food than they would be with adequate sleep.
Sleep disruption compounds weight gain through:
- Elevated ghrelin (hunger hormone) — increasing appetite, especially for high-carb, high-fat foods.
- Reduced leptin (satiety hormone) — making it harder to feel full.
- Increased cortisol, as the body attempts to compensate for fatigue with stress hormones.
- Impaired insulin sensitivity — promoting fat storage from carbohydrate intake.
- Reduced willpower for food decisions — not a character issue, a prefrontal cortex fatigue issue.
What About Inflammation?
Depression is now understood to involve a significant inflammatory component. JAMA Psychiatry and related research have identified elevated inflammatory markers (particularly C-reactive protein and interleukin-6) in people with depression, and chronic low-grade inflammation is independently associated with obesity, insulin resistance, and impaired leptin signalling.
This means depression and excess weight share overlapping biological drivers, creating a cycle where each condition can worsen the other at a physiological level.
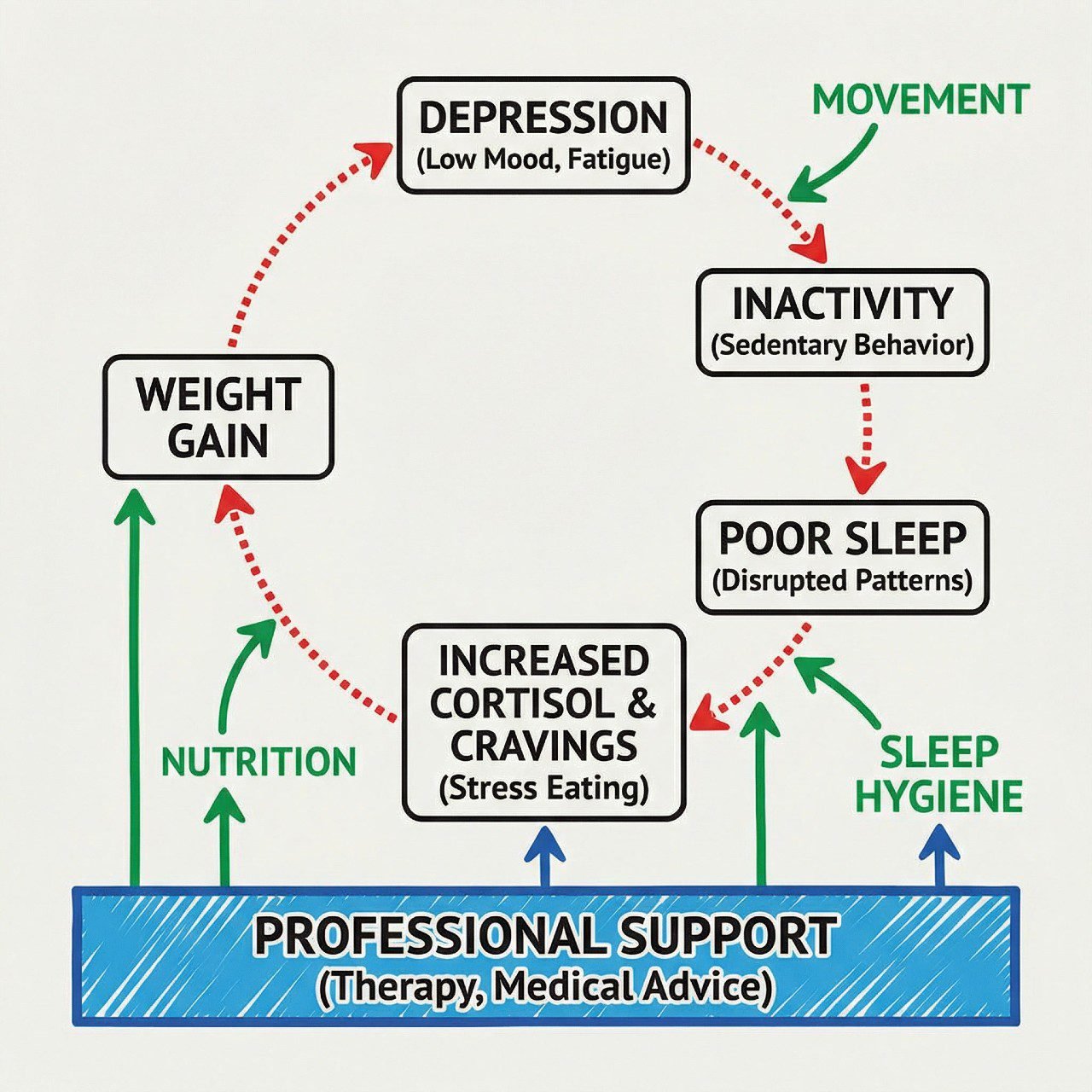
How to Break the Depression-Weight Gain Cycle
Breaking the depression-weight gain cycle requires addressing both systems simultaneously — starting with the smallest, most sustainable interventions and building from there. Trying to "fix" weight while ignoring depression, or treat depression while ignoring weight, leaves half the biological cycle intact.
Small, Compassionate Steps That Work
The most important word here is small. When you're living with depression, the gap between "I know what I should do" and "I can actually do it" can feel enormous. Strategies that work here respect that gap — they don't try to jump over it.
Practical interventions with evidence behind them:
- Omega-3 supplementation — a low-effort, high-return first step. A 2019 meta-analysis in Translational Psychiatry found that omega-3 supplementation significantly reduced depressive symptoms
- 10 minutes of daily outdoor movement — the combination of light, movement, and nature reduces cortisol measurably
- Protein at every meal — stabilises blood sugar, reduces cortisol-driven cravings, and supports serotonin precursor production (tryptophan is found in protein-rich foods)
- Consistent sleep and wake time — even without perfect sleep quality, a consistent schedule anchors the circadian rhythm and reduces the cortisol spike that comes from irregular waking
- One stress-reduction practice — meditation, breathwork, journalling, or therapy. Any of these, done consistently, lowers chronic cortisol over time
- Reducing alcohol — alcohol is a depressant, worsens sleep quality, and directly promotes fat storage. Reducing it is one of the highest-leverage steps possible for both mood and weight
On building emotional wellness habits: Using Mindfulness to Break the Cycle of Emotional Eating →
When to Seek Professional Support
This article gives you tools and understanding. It is not a replacement for professional care.
Consider seeking support from your GP or a mental health professional if:
- Depression has persisted for more than two weeks.
- You are experiencing significant changes in appetite, sleep, or weight.
- Thoughts of self-harm or hopelessness are present.
- Your daily functioning — work, relationships, basic self-care — is significantly impaired.
Types of support that have evidence for both depression and weight management:
- Cognitive Behavioural Therapy (CBT) — shown in multiple trials to reduce both depressive symptoms and emotional eating patterns.
- Registered dietitian consultation — particularly valuable if medication-related weight gain is a concern.
- Exercise psychology or physiotherapy — for a structured, supported return to movement at any capacity level.
- Support groups — reducing isolation is itself a therapeutic intervention.

A New Perspective on Depression and Your Body
When depression causes weight gain, the most harmful thing is the story we tell ourselves about it.
I have no self-control. I'm weak. I should be able to manage this. Everyone else can. What's wrong with me?
None of that is true. And more importantly, none of it is useful. Those stories deepen the very depression that is driving the biological changes you're experiencing.
The truth is more complex and more kind: your brain is managing an illness, and your body is responding to that illness. The weight is not a moral statement. It is a physiological signal.
Understanding the four — now five — mechanisms behind depression-related weight gain doesn't just educate you. It reframes the problem from "I keep failing" to "I have a system that needs supporting." And from that place, small, consistent action becomes possible. That is where transformation begins.
Related Articles
The Bottom Line
Depression and weight gain are connected through biology — not willpower. The four core mechanisms are:
- Motivation depletion — a neurobiological symptom that makes physical activity genuinely harder.
- Chronic cortisol elevation — directly promoting fat storage, cravings, and abdominal weight gain.
- Medication side effects — a documented reality to discuss openly with your doctor.
- Nutritional deficiencies — depleting the very nutrients that metabolism and mood depend on.
Add sleep disruption and inflammation, and you have a complex, interlocking biological system — not a personal failing.
The path forward is compassionate, systematic, and grounded in understanding your body rather than fighting it. Small steps, professional support where needed, and the knowledge that biology is workable, even when it feels overwhelming.
Embrace Inspiration:
Like What You Read? Be Sociable, Comment, And Share It! Thanks.
Glossary Of Key Terms
FAQ
Yes. Depression causes weight gain through several documented biological mechanisms: elevated cortisol driving fat storage and cravings, reduced physical activity from neurological motivation depletion, sleep disruption raising hunger hormones, nutritional deficiencies impairing metabolism, and — in some cases — weight gain as a side effect of antidepressant medication. This is physiology, not a lack of effort.
Chronic cortisol elevation — a hallmark of depressive states — directs fat storage preferentially to the visceral (abdominal) region. Cortisol also reduces insulin sensitivity and amplifies cravings for high-sugar, high-fat foods. In women approaching perimenopause, the declining protective effect of estrogen makes this abdominal fat accumulation more pronounced.
No — weight gain risk varies significantly between medication classes and individual drugs. Some antidepressants (particularly certain SSRIs and TCAs) are more associated with weight gain; others have a neutral or even weight-reducing profile. If you are experiencing weight gain you suspect is medication-related, speak to your prescribing doctor. Never reduce or stop antidepressant medication without medical supervision.
Yes, with appropriate support and realistic expectations. The most effective approaches address both the depression (through medical care, therapy, and lifestyle) and the specific biological drivers of weight gain (nutrition, gentle movement, sleep, stress reduction) simultaneously. Expecting standard diet-and-exercise approaches to work while depression goes untreated overlooks the biology. Treating the root cause creates the conditions for sustainable change.
Yes. Depression affects individuals differently — while many experience weight gain through the mechanisms described above, others lose weight due to significantly reduced appetite, disinterest in food, or nausea. Both responses reflect the same underlying disruption to appetite and reward regulation. Significant unintentional weight change in either direction warrants medical evaluation.
Foods that simultaneously support mood and metabolic health offer the most value. Prioritise omega-3-rich fish (salmon, mackerel, sardines) for inflammation and brain function; leafy greens for folate and B vitamins; protein at every meal to stabilise blood sugar and support serotonin precursors; and whole grains for sustained energy without blood sugar spikes. Reducing ultra-processed foods, alcohol, and high-sugar snacks removes the primary drivers of cortisol-related fat storage.
Join Our Mailing List
Ready to build a foundation for both mental and physical wellness? Download the free Lean Body Formula Special Report — 10 evidence-based strategies for permanent fat loss, designed specifically for the female body.

I really loved this article because being a coach in the health and fitness industry for over 16 years, it’s literally last year I discovered the link between depression and weight gain. Since tackling the depression and emotional triggers first I’ve found I can deliver results way faster than before. Great article 👍🏿
Thank you, Rasheed. I hope it helps!